On April 6 the White House announced a Health Alert Network (HAN) advisory warning about the effects of medetomidine, an unregulated sedative that has been increasingly found mixed with fentanyl. The HAN was jointly issued with the CDC, which announced it several days earlier. This appears to be the first time that the federal government has used this type of alert to warn about the unregulated drug supply.
Medetomidine began gaining notice in the East Coast drug supply in 2024. It can be thought of as the direct successor to xylazine, the unregulated veterinary tranquilizer that emerged a few years earlier but has recently diminished as various levels of government attempt to control the supply by way of harsher enforcement. Xylazine in combination with fentanyl was designated an “emerging health threat” by the Biden administration in 2023, and xylazine itself is currently on the cusp of being banned under Schedule III of the CSA. Predictably, targeting xylazine in this way has pushed the drug supply toward alternatives that are even less familiar.
“The public health community, as well as those who put themselves at risk of overdose due to illegal drug use, need to be aware of ever-evolving dangers,” stated Director of National Drug Control Policy Sara Carter in the White House announcement. “Medetomidine represents a real threat to communities, and this once again reaffirms that the only safe level of illegal drug use is zero.”
The CDC usually issues HAN every few weeks or so, but historically these have focused on disease outbreaks. There have been no HAN related to fentanyl or xylazine, for example. The only prior HAN to discuss overdose or banned drugs was a 2024 alert warning that overdose risk could increase as a result of patients losing access to prescription stimulant medications like Adderall.
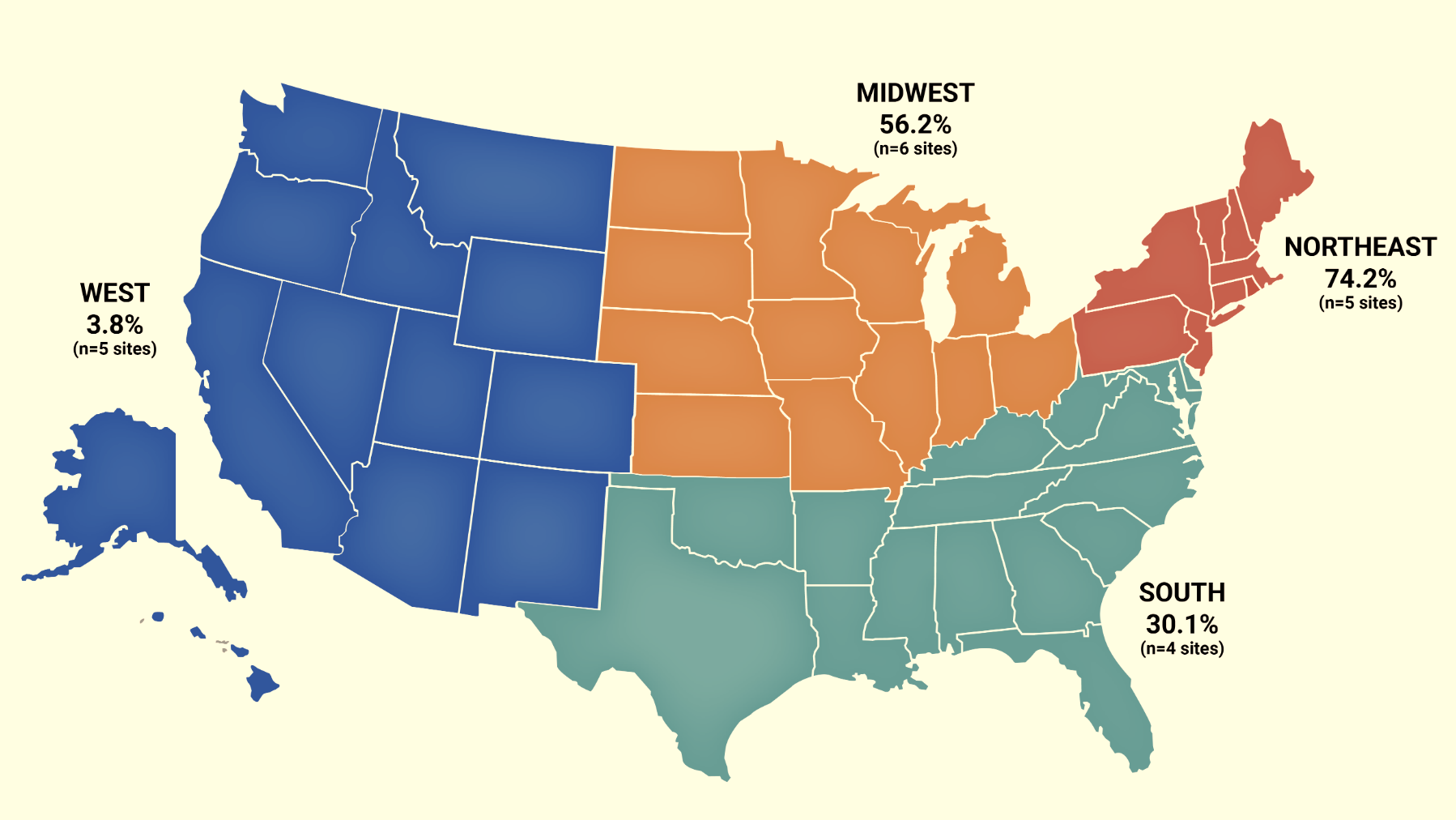
The CDC stated that law enforcement drug seizures appeared to show medetomidine becoming increasingly prevalent. It was identified in 247 seized drug samples in 2023; then 2,616 samples in 2024; then 8,233 samples in 2025. Geographically, these samples have been concentrated in the Northeast, with very few samples identified in the West.
However, this still represented less than 1 percent of samples reported to the National Forensic Laboratory Information System in 2025. While the general consensus among public health experts is that medetomidine’s presence in the supply has been increasing, it should be noted that this kind of exponential uptick in detected samples always happens once a new substance attracts media attention and more laboratories start to check for it.
Outside of laboratory settings, there are also medetomidine test strips that work similarly to the better-known fentanyl test strips. Erin Tracy, lead chemist at the UNC Street Drug Analysis Lab, said that medetomidine test strips appear to be very sensitive—even compared to test strips for fentanyl or xylazine, which can detect those substances in very low quantities. This makes them potentially much more useful to people who use fentanyl than fentanyl test strips, which are often somewhat purposeless in this context.
Medetomidine is not associated with soft-tissue infections that often follow xylazine injection. But it has distinct side effects of its own.
As medetomidine and xylazine are similar, so are some of the effects associated with them—namely prolonged sedation, which can persist even after naloxone has restored independent breathing. Though all that’s necessary to reverse an opioid overdose is for the person to be breathing on their own again, the mistaken belief that they need to “wake up” can lead to administering more naloxone than was necessary.
Medetomidine is not associated with the soft-tissue infections that often follow xylazine injection. But it has distinct side effects of its own, most notably a withdrawal process that can be much more damaging than withdrawal from opioids alone. This is marked by rapid heartbeat and high blood pressure and can require intensive hospitalization.
The withdrawal symptoms can be mitigated with IV infusions of medications like dexmedetomidine, the more potent of medetomidine’s two isomers, which unlike medetomidine itself is FDA-approved as a sedative that can be used in hospital settings.
“Withdrawal can be so severe that [experts] advise going to ER where staff have been oriented to manage medetomidine withdrawal,” Maya Doe-Simkins, co-director of naloxone-access group Remedy Alliance, told Filter. And “encouraging people who want to detox to do it at a hospital, versus regular detox.”
Though media and law enforcement have widely described non-opioids like medetomidine as “naloxone-resistant”—a misleading label that is always useless at best and harmful at worst—it’s not entirely clear whether it’s accurate in this case. There’s emerging evidence that xylazine responds to naloxone, and we haven’t established yet that medetomidine doesn’t act similarly. But the more relevant point is that since medetomidine is almost always found with fentanyl, naloxone can still help reverse overdose.
Doe-Simkins said that for people responding to overdose in regions where medetomidine has been identified, the standard best practices for naloxone administration still apply—ideally using intramuscular naloxone to start with a low dose and titrate up if needed, with the emphasis on rescue breathing rather than potentially giving someone more naloxone than necessary.
Image (cropped) via Centers for Disease Control and Prevention