Traditionally, the conversation around US safe supply consists of saying that we don’t have one and then pointing to Canada. Even the most constrained and medicalized models of safe supply feel so far away. A lot of this is because we have a Drug Enforcement Administration where there could be just a health department, but one of the quieter things holding us back is that we have very little public access to forensic drug-checking technology.
Only a handful of harm reduction programs in the US have the expensive spectroscopy instruments that can analyze a drug sample and tell you what’s in it, so anyone who doesn’t live in their vicinity pretty much has to guess. Drugsdata.org has a mail-in program that accepts samples anonymously, but it’s unwieldy and expensive and the results take several weeks.
Various public health pilots documenting supply changes are building the evidence base that will be used to push safe supply at the policy level, but that’s years away. Meanwhile, most of what we know about our supply comes from law enforcement seizures and postmortem toxicology reports. None of these are any good to the people trying to survive the illicit supply right now. We need something we can use while we’re still alive.
Drug checking an unregulated market only goes so far. But it can allow people to use the current supply more safely, which is what I’ve seen happen with a new mail-in program out of North Carolina. They send you a kit, you send it back with a residue sample, and within a day of its receipt you know what was in it, including fillers. You remain anonymous, and spend $0.
For the past month or two, while the kits have still been in development, I’ve been using them to submit samples from participants at the NYC syringe service program (SSP) where I’m a peer worker. The kits are now rolling out across the US, marking the beginning of our first free, rapid national drug-checking service.
How It Works
Each kit has a vial of methyl cyanide, which denatures your sample so that from a DEA standpoint nothing in it can be considered a controlled substance. According to Dasgupta, this makes it legal to distribute through the mail. Research labs do the same thing for commercial products, it just hasn’t been used for public health before.
You can drop in a few specks of powder, but swabbing the inside of an empty bag with a Q-tip will work even if there’s no visible residue. I’ve gotten results from glass containers that looked spotless and wax paper bags with nothing left in the creases. You can also just drop in cottons after you’ve used them.
There’s an optional response card that asks basic identifying questions about the sample, but none about you. The whole process takes maybe a minute and a half, plus dropping it off at the post office or FedEx. Each kit comes with everything you need to use it including a prepaid shipping label and a pencil..
Once your sample arrives at the Core Laboratory at the University of North Carolina, it’s analyzed with gas chromatography mass spectrometry (GC-MS), sometimes in combination with Fourier transform infrared (FTIR) and fentanyl immunoassay strips if the situation calls for them.
Even for the harm reduction programs with access to FTIR, confirmatory GC-MS testing—often the only way to ensure accuracy, especially with complex samples—can take weeks.
The team is already fielding requests from programs in California, Indiana, Michigan and Georgia.
Dr. Nabarun Dasgupta, who developed the program along with Maryalice Nocera (logistics and kit design) and Mary Figgatt (data analysis), spent much of the pandemic streamlining the turnaround to just two days. Recently the team was joined by chemist Erin Tracy, who defected from her job at a government crime lab and has gotten the process from two days down to one. The lab has a DEA license, so the team has authorization to handle controlled substances, along with the benefit of a lot equipment in one place. They’ve tested around 150 samples so far.
Dasgupta has actively solicited and incorporated feedback as I’ve sent in samples and interpreted the results with participants, but the program has been informed since the beginning by members of the North Carolina Urban Survivors Union, so the kits were already highly optimized way before we joined up.
In early March, the team received grant funding from the Foundation for Opioid Response Efforts (FORE) to collaborate with SSP. The funding allows them to begin the first state-wide public health assessment of street supply, for which they’ll work with seven programs across North Carolina. But it also means they can begin sending kits to SSP in other states.
They’re already fielding requests from programs in California, Indiana, Michigan and Georgia. More are reaching out by the day, so the process of scaling up is something they’re figuring out in real time.
“You were one of our first pilots, and since we’ve sent your stuff we’ve had five or six other requests,” Dasgupta told Filter. “And so we were like, we really need to turn this into a service that’s easy and cheap, which I think we can do.”
How to Use Your Results In the Real World
The DEA still stands between us and the most critical information we can learn from spectroscopy checking, which is purity—what percentage each compound is of the sample’s overall weight. If you know that the dope you usually get is, say, 10-15 percent fentanyl, or that a bag you overdosed on was 20 percent fentanyl, then you have an idea of where your tolerance is and what’s safe for you.
“Law enforcement [told us] that if you assign purity to a sample, then that is quote-unquote ‘quality control for drug dealers,’” Dasgupta said, describing the ideal outcome for everyone except law enforcement. DEA-licensed labs are forbidden from sharing quantitative data with the public even if they had it.
The peaks you’ll see in your results aren’t related to purity anyway; they’re more to do with the distribution of molecules throughout a sample, and any reading of them is somewhat subjective. This is especially true for similar compounds like fentanyl and fentanyl analogues, whose peaks might overlap. But even though the peaks don’t indicate percentage by volume, their relative heights do give you a sense of whether there’s a lot of something or a little.
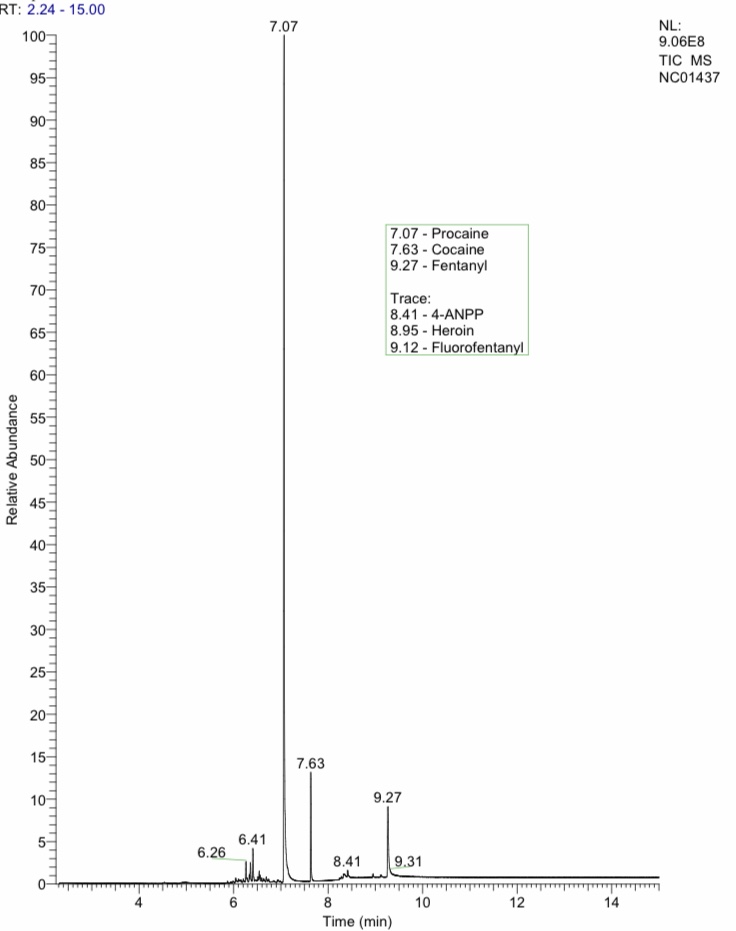
Something I hear consistently from people in one particular neighborhood is that they keep getting dopesick because the supply is so weak that some days they can’t even feel it, not just the $5 bags but the regular $10s too. Which makes sense, because what they’re injecting is mostly procaine, the local anesthetic commonly used for dental work.
All dope samples I’ve sent have contained fentanyl, which isn’t news to anyone, least of all the people who provided them. But fentanyl isn’t the only adulterant, and overdose isn’t the only harm.
Everyone who contributed samples knew the gist of what their heroin is these days—fentanyl bulked out with various fillers—but none of them had ever known which analogues or which fillers. Besides fentanyl, samples I’ve sent have been cut with fluorofentanyl, phenethyl 4-ANPP/despropionyl fentanyl, 6-MAM, xylazine, tramadol, cocaine, procaine, noscapine, caffeine, quinine, sucrose and phenacetin. Sometimes there’s heroin, too.
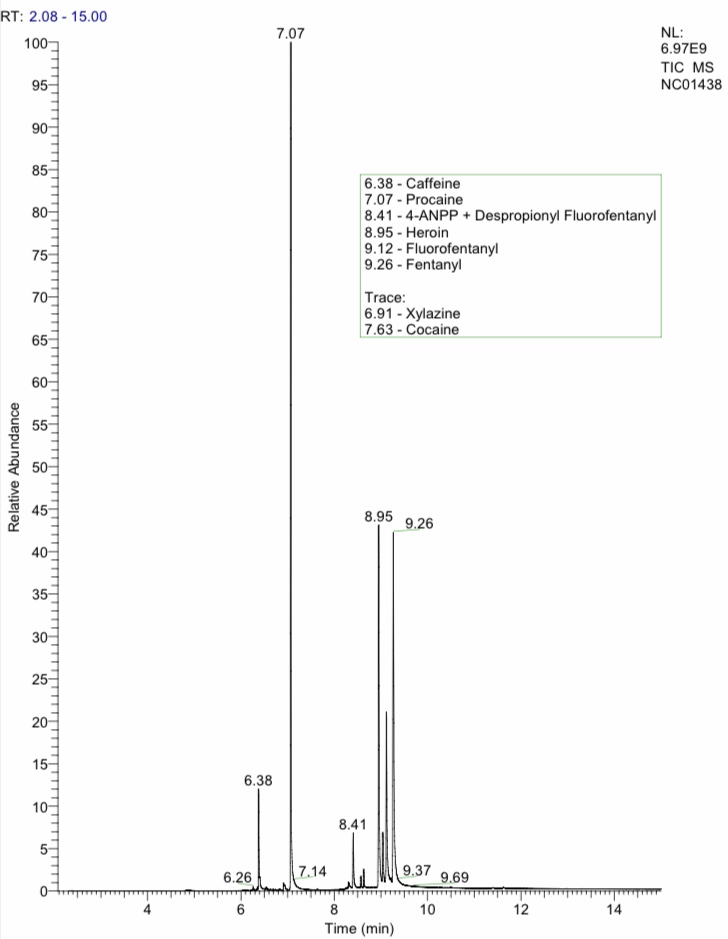

The two samples above were the same stamp, purchased from the same seller on the same block on the same day. They’re identical for procaine and heroin, and besides fentanyl have half a dozen of the same overlapping analogues and fillers. But the first one has a lot more fentanyl, plus it steered the conversation toward xylazine.
The amount of xylazine looks tiny, and the person who’d used that bag hadn’t noticed anything off. But when I described xylazine’s effects, they instantly connected some of them—entire arm stiff like dead wood; abscesses that hadn’t made any sense; falling out quickly, with no warning—to two bundles from that same seller within the past year.
Now they know to look out for dope that cooks up darker or has a strong smell, and that those are the shots where it really matters to anchor the vein, inject as precisely as possible and leave the needle in for a bit to minimize leak into the surrounding tissue. In real life they probably won’t always be able to take the time, but they carry tourniquets now.

This was the only heroin sample I’ve sent so far that actually deserved the name. Thankfully, none of the other crap in there was noticeable enough to ruin the bag for the person who submitted it. They’re fortunate to have continued access to the same seller, and plan to use them exclusively.
Probably the most impactful use of the results, especially over time, is that all of us are relaying them back to the sellers.
I didn’t focus on cocaine and meth solely because those results wouldn’t mean much to the specific people I work with, but the kits work just as well for those too.
My meth is just the one ingredient, which is nice to know but doesn’t change anything. Pure meth still isn’t that uncommon, and it’s not the drug of choice for most people where I live anyway.
I sent a cocaine sample I suspected would check out as cocaine, and it did, but even that’s only been useful to maybe two people; everyone else I know uses it to speedball and does something like 1:2 cocaine to dope, so ensuring that their tiny bit of cocaine doesn’t contain a tiny bit of fentanyl isn’t a huge priority.
Scaling Up
Everything the team produces will be open source, and all the sample results will be public. The interface is still being built out but will be along the lines of drugsdata.org, just a bit more readable and less techy. None of the data will ever be shared with law enforcement or used as evidence in court.
As the service evolves, Dasgupta is eyeing its potential as an effective drug alert system in the immediate aftermath of any mass overdose.
“I want to have this be like a rapid response kind of thing, where we can just drop a few dozen kits in that area right now and get results back out in a day,” he said. “What would it take to build that?”
Right now the team’s capacity is around 2,000 kits per year, so they’re currently only supplying them to SSP. They can keep the turnaround under two days even if they expand beyond SSP, but the main barrier is funding. Each kit is about $2 in materials; $18 once you factor in machine processing time. Then there’s shipping and labor. The grant only takes them so far, so they’re looking for ways to recoup some of the costs.
“We were totally bootstrapping this,” Dasgupta said of the year and a half leading up to the FORE grant, during which he mostly covered the costs himself. “What we have is clearly a process that works, and the capacity to do it, [but] we need to make more kits and we need to figure out how to pay for them.”
Feature art by Brooke Alexandria Paine