[This article contains an image of injection wounds.]
I had my first injection infection in the winter of 2020. I knew that they were much more common than most people thought, but for the longest time I hadn’t practiced what I’d preached. Swabbing before injecting? Who actually did that?
The infection appeared on my right leg, from the top of my calf to my inner thigh. It hurt, but I had no other good veins to inject. When friends saw the infection, they were worried I could lose my leg.
Before this, the closest I’d had to an injection-related infection were a few bad abscesses. So I called Rick the Nurse—a famous Canadian street nurse from Halifax’s Mobile Outreach Street Health (MOSH). Rick, who’s been serving the underserved in Halifax for more than a decade, knows practically every person living on the street who uses drugs, and once a week he pairs up with Mainline Needle Exchange to go out and meet people where they’re at. Everyone knows Rick the Nurse.
Rick quickly diagnosed me with cellulitis, a common bacterial skin infection, and wrote me a prescription for antibiotics.
Rick the Nurse is a tall gentleman, always wearing an amazing fedora. He’s the kind of person a lot of us could chat with all day. He knows when to listen and when to talk, when to laugh, and when to stay quiet and make space for whatever each patient is going through. After years of working with Rick in our field, this was my first time seeing him as a patient.
I thought maybe my infection had something to do with all the pure cocaine I was using. It certainly seems like that might be the reason; Rick said that with cocaine injectors he does tend to see more cellulitis than abscesses.
“I tell someone to heat it, calm down on it for a little bit,” he told me. “Then I check back in a couple of days and sometimes it’s gone.” But “sometimes it’s [turned] into cellulitis, meaning that the cells are now infected.”
Rick quickly diagnosed me with cellulitis, a common bacterial skin infection, and wrote me a prescription for antibiotics. He told me that I would not lose my leg. Within a week, I was all healed up, even though I was still injecting.
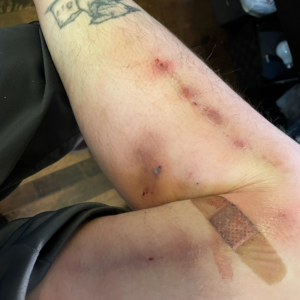
I had never really understood the difference between different kinds of infections. An infection was just an infection to me. Rick was the one who explained to me what cellulitis was. Bacteria gets into your bloodstream, transferred there from the surface of your skin during the injecting process—often when you don’t take the step of swabbing the injection site with alcohol. And cellulitis can lead to endocarditis.
Endocarditis—a heart infection that can result from injection-related infections—is set to kill one out of every five people who inject opioids by 2030. It is under-researched, and overrepresented among the most marginalized drug users—the people who aren’t always able to wash their injection site before they hit, such as those without housing or regular access to showers.
Since my first cellulitis infection, I’ve had a few other close calls—bad misses on my feet, or open injection wounds not healing properly. MOSH has continued to provide me with helpful tips and tricks—asking me to feel the area in question to see if it was hot, or circle the area with a Sharpie to see whether it’s growing larger.
I’m still an injection drug user, just a bit safer and wiser now. We all benefit from practicing harm reduction techniques when using drugs—using sterile supplies every time, swabbing with alcohol prior to injecting, rotating veins to help avoid abscesses and infections.
Criminalization pushes drug users to the outskirts of society—places where hygiene products are as rare as brand new sterile syringes. We need people who use drugs—the experts in this field—to share their knowledge with those who haven’t had access to this knowledge, who will never be helped by traditional doctors who don’t practice harm reduction and won’t even explain in layman’s terms what’s going on. We need this education passed on so that everyone, from the most privileged to the most marginalized, stands half a chance at surviving—whether that means being saved from an overdose or from catching a potentially deadly infection.
Top photograph via City of Raleigh, North Carolina. Inset photograph by Matthew Bonn.