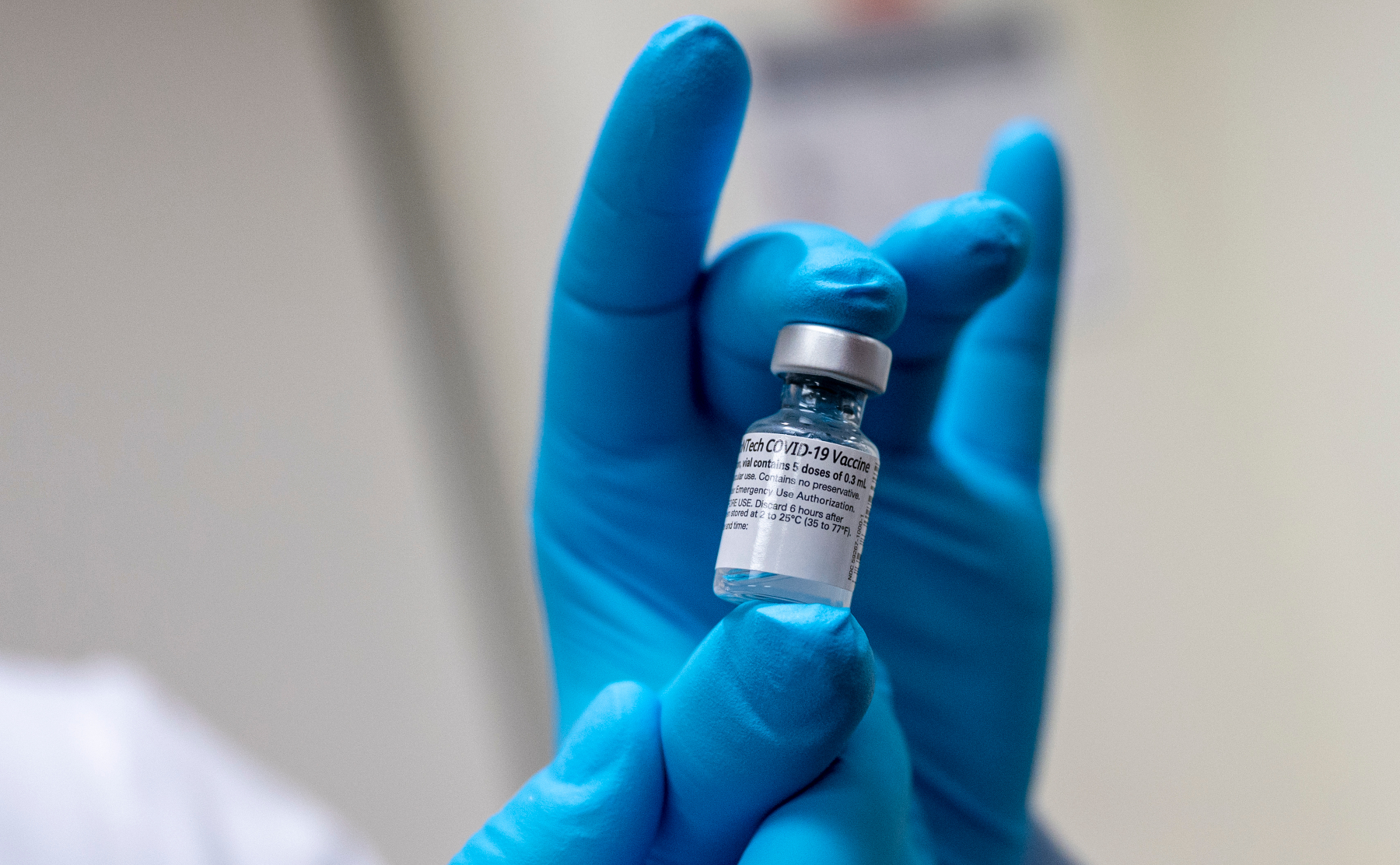
Millions of Americans are happy to finally be venturing out of their quarantine cocoons, emboldened by newly minted COVID-19 vaccine cards and updated CDC mask guidance.
But not so fast. The Biden administration has officially missed its target of vaccinating 70 percent of adults by July 4, with less than half of the population fully vaccinated at publication time. And as the highly contagious Delta variant continues to spread across the US, cases and hospitalizations are on the rise in most states, especially those with low vaccination coverage. That leaves many people and communities at risk—disproportionately the most marginalized communities, including people who use drugs.
A study released back in September confirmed what others had noted earlier in the pandemic and did again subsequently: People who use drugs, especially opioids, are more likely than the general population to be hospitalized and die from COVID-19. Compounding these risks are conditions known to co-occur with substance use disorders, including mental health issues, HIV and chronic liver disease.
As we have learned, the effects of the virus have reached far beyond its physical symptoms. The chronic stress, isolation, and uncertainty of the pandemic have resulted in a mental health crisis, marked by increases in depression and binge drinking, and a staggering 50 percent increase in overdose deaths—with 2020 bringing the highest number of such deaths ever recorded in US history. Many of these deaths involved opioids, including fentanyl, but stimulants including cocaine and methamphetamine have also contributed. Add on a strained health care system that was already struggling to keep up with the crisis of addiction and overdose, and the result is more suffering and death for those who were already vulnerable before the virus entered our lives.
“I know many friends that haven’t gotten the vaccine. People who use drugs are reluctant to engage with the health care system for good reason.”
“I have no doubt that there are countless untold stories of people that use drugs dying as a result of COVID-19—either from the virus itself or from reduced access to lifesaving support like methadone or syringe service programs,” Aaron Ferguson told Filter. Ferguson is on the leadership team of the National Urban Survivors Union, an organization that represents people who use drugs seeking to undo US prohibition policies.
“I know many friends that haven’t gotten the vaccine,” he added. “People who use drugs are reluctant to engage with the health care system for good reason. Most of my fellow drug users have experienced discrimination in health care settings ,and may have experienced severe consequences for seeking medical care due to mandated reporting that can result in losing our families, communities and livelihood.”
Unfortunately, despite the work of advocates like Ferguson, efforts to support drug users have fallen short during the pandemic. The CDC only recently acknowledged substance use as an underlying health condition that should be prioritized for vaccination.
Dr. Nora Volkow, the director of the National Institute on Drug Abuse, agrees with the prioritization and is frank about the risks at hand. “Getting the COVID-19 vaccine is crucial for substance use populations because they have a much greater likelihood of having severe outcomes from the virus, including death,” she told Filter.
“The risk might be due to an increased likelihood of underlying medical conditions, reduced access to health care, or increased chances of living or using drugs in group settings,” she continued. “The acute effects of drug use might also complicate the signs and symptoms of the virus. For instance, breathing difficulties can be exacerbated by opioid use.”
No study to date has examined whether vaccination rates differ depending on a person’s drug use history. But we do know with great confidence that no matter who you are, the vaccine can save your life. On July 4, Dr. Anthony Fauci announced that over 99 percent of recent COVID-19 deaths in America have involved unvaccinated people.
So, what is being done to support people using drugs as we navigate the next stages of COVID and the vaccine rollout?
“The messengers matter as much as the message.”
One promising effort is a collaboration between the Addiction Policy Forum (APF) and Foundation for Opioid Response Efforts, called the “Vaccine Navigator Initiative.” The program increases outreach to people who use drugs (and caregivers) by answering questions and providing information about COVID, the vaccine, vaccination sites and other support services. The “navigators,” which include social workers, certified drug and alcohol counselors, and peer engagement specialists, can be reached through an online form or by phone/text at 833-301-HELP.
Jessica Hulsey, APF’s CEO, emphasizes the importance of trust in the Vaccine Navigator Initiative. “The messengers matter as much as the message,” she told Filter. “Utilizing peers, trained individuals in recovery from substance use disorder, to discuss vaccinations, answer questions and help clients with any other challenges is key.”
Trust is a concept central to the larger conversation about vaccinations and relates to the severe barriers that people who use drugs face in navigating health care systems, as noted by Ferguson. In a recent study, there was evidence that treatment was withheld from patients diagnosed with COVID-19 when those patients also had chronic liver disease and a history of alcohol use disorders. The consequences of this biased care were devastating, with 80 percent of these patients ultimately succumbing to the virus.
This type of stigmatization can understandably erode trust in health care providers. And when it comes to COVID vaccination, one survey study found that at least a quarter of people with current or past substance use disorders were unwilling to get the vaccine due to distrust.
Phillip Rutherford, chief operating officer at Faces & Voices of Recovery, sees vaccine access and distribution as the more pressing issues, echoing nationwide concerns about inequities in vaccine distribution. “You have to meet people where they are out in the community,” he told Filter of vaccination efforts. President Biden made just this point on July 6 when he highlighted the importance of mobile vaccination clinics.
For the most part (with some exceptions), COVID-related outreach in the substance use community has focused on providing information rather than the vaccine. However, it could be that mobile vaccination—similar to programs in Boston for people experiencing homelessness and in Baltimore for aging adults—could be tailored to reach people who use drugs and want to get the vaccine. Likewise, there could be unmet opportunities to embed vaccine education and administration efforts into existing infrastructures that support people who use drugs, including methadone clinics or community treatment centers. I was unable to locate any widespread COVID vaccination programs utilizing these strategies.
For Dr. Josh Barocas, assistant professor of medicine at Boston University School of Medicine/Boston Medical Center and the author of an editorial on this issue in the New England Journal of Medicine, the lack of tailored vaccine efforts is less about motivation and more about competing priorities.
“I suspect that while organizations may want to provide additional services such as vaccines, the issue is about capacity and resources.” he told Filter. “We are dealing with upticks in HIV and hepatitis C among people who inject drugs as well as a surge in overdoses. Because of resource limitations, service programs have to prioritize, and without additional resources, they are likely unable to add vaccines to the long list of services they are providing.”
“If someone comes in looking for harm reduction supplies and information, and you are coercing them into getting vaccinated, that is not harm reduction.”
That raises questions about support for harm reduction itself. Because if resources and time are going to be invested into the programs focused on the COVID vaccine among people who use drugs, then shouldn’t we be investing the same time and resources into other life-saving, evidence-based interventions, including syringe service programs, safe consumption sites, naloxone distribution and medications for opioid use disorder?
“I believe every opportunity to talk to people who use drugs is a good time to discuss the impacts of fentanyl, overdose prevention, syringe service programs and yes, the COVID-19 vaccines as well,” Mike Selick, associate director of capacity building at the National Harm Reduction Coalition, told Filter. “The issue here is how programs treat people rather than the services being combined. If someone comes into your organization looking for harm reduction supplies and information about how to use drugs more safely, and you are pushing them and coercing them into getting vaccinated, that is not harm reduction.”
Selick offers an important reminder that starting from a place of respect, listening and consent is essential if trust is to be built—supporting people who use drugs in making informed decisions about their own health, whether that’s a COVID vaccine or harm reduction and treatment resources.
Ferguson’s lived experience as a drug user reinforces this point. “COVID vaccines could be an opportunity to engage people who use drugs in the health care system in a non-stigmatizing way and as an entry point to other types of care,” he said. “Otherwise such efforts will continue to be disproportionately offered and serve as yet another reason for us to distrust health care.”
With the vaccine rollout continuing, the risks of COVID ought to subside further as the year moves on. But the risks of using drugs from an adulterated, unregulated supply will not. It’s vital that we learn the lessons of these times—about the need for equitable access to health resources and the need to empower people who use drugs through many options and resources, not just those related to COVID.
Photograph by US Secretary of Defense via Wikimedia Commons/Creative Commons 2.0