As the already-staggering death toll of the overdose crisis reaches historic heights, the United States’ premier public health agency called for services that check participants’ drug supplies, an unexpected endorsement for a federal government that’s historically been hostile toward harm reduction policies.
In a December 17 health advisory, the Centers for Disease Control and Prevention (CDC) recommended—for what appears to be the first time in its history—the establishment of drug-checking programs by harm reduction organizations in order to “[i]mprove detection of overdose outbreaks” involving illicit drugs commonly adulterated by fentanyl, a potent synthetic opioid, novel psychoactive substances and benzodiazepines. In harm reduction circles, drug-checking is a tool used to promote the bodily autonomy of people who use drugs.
“I think this is a positive sign and an implicit acknowledgment of several things,” Dr. Sheila Vakharia of the Drug Policy Alliance* told Filter. “One, the adulterated drug supply driving the overdose crisis rather than regulated prescription opioids. Two, the research base behind the utility of drug checking technologies. And three, that people who use drugs want to know what is in their drugs and are capable of making informed choices about their drug use.”
The CDC appears to be moving, at least in part, past a major barrier currently obstructs local harm reductionists interested in providing drug-checking and similar services: drug paraphernalia criminalization. Federal law threatens imprisonment of up to three years for paraphernalia possession. Agency heads have expressed hostility towards such harm reduction tools. Leadership for the Substance Abuse and Mental Health Services Administration, another federal health agency, has outright denounced them.
The CDC appears to be moving past a major barrier: drug paraphernalia criminalization.
Some states, like Maryland, have exempted drug checking kits from their paraphernalia statutes. Many still do not, as the CDC appears to recognize in its statement that drug-checking services must be operated “in line with applicable state and local laws.”
For Vakharia, the agency could play an advocacy role in lifting this barrier. “If the CDC wants to more actively support the establishment of drug checking services, they should also endorse changes to those laws that would allow drug checking services to exist in more places,” she said.
Currently, the range of institutionalized US drug-checking services pales in comparison to what’s offered by organizations in Canada and some western European countries. The Centre for Drug Policy Evaluation in Toronto uses lab-based technologies, like mass spectrometry, to assess samples submitted by participants at the city’s safe consumptions site. It’s able to identify each substance present in a sample and approximate quantities, regardless of a participants’ suspicion.
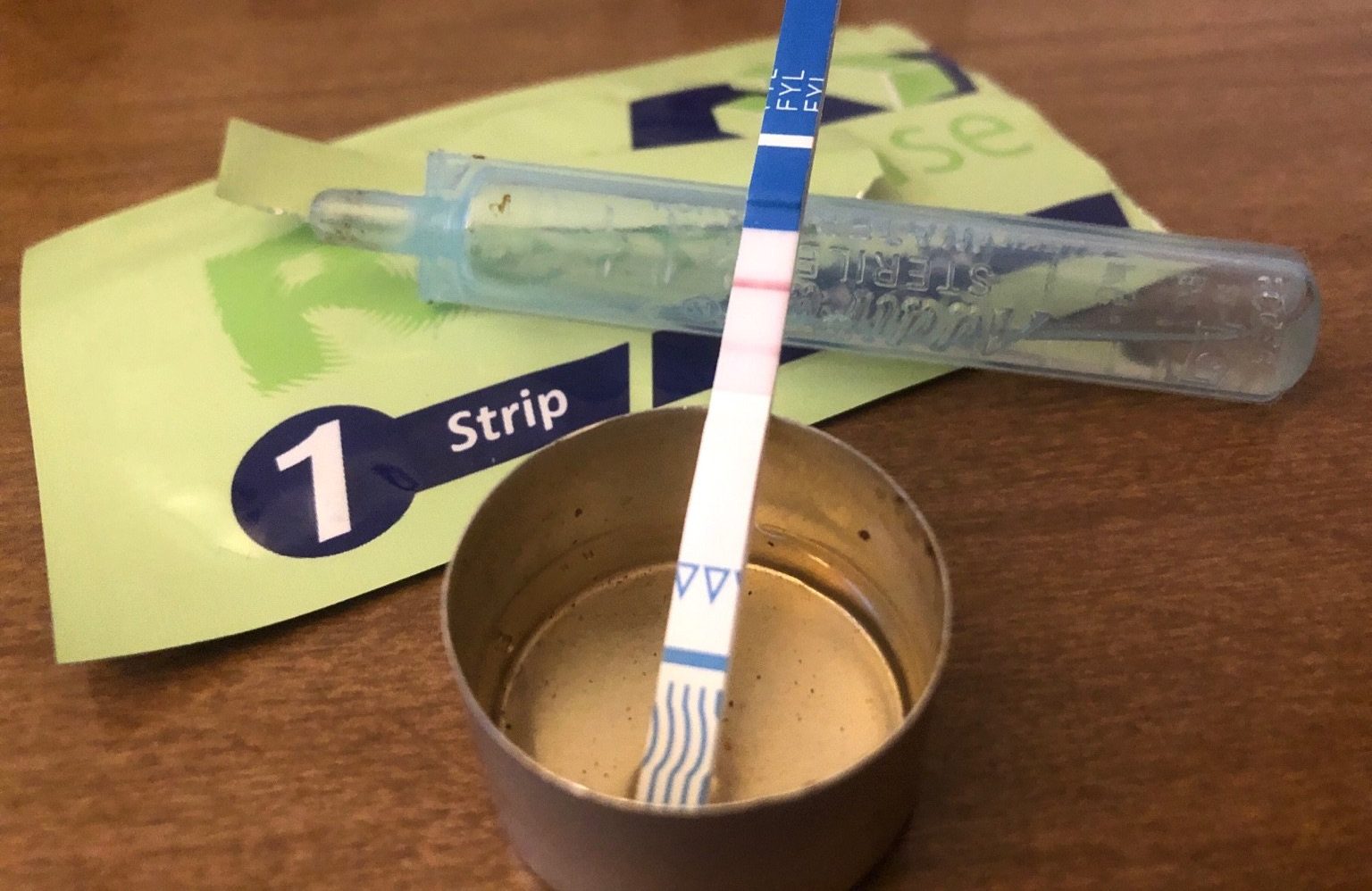
In contrast, drug-checking tech usually used in the US tends to require a participant check for a specific substance. Such is the case with fentanyl test strips, thin paper strips designed to check urine for the synthetic opioid. Researchers found fentanyl test strips to be cost-effective and highly accurate tools for detecting the adulterant that’s driving the country’s unprecedented overdose death toll.
But the strips, which are increasingly distributed by syringe service programs to their participants, “are no panacea,” Norwegian researchers wrote in a December 2020 study, since they fail to detect some fentanyl analogues. That presents a problem in an ever-changing drug supply forced to adapt to the US-led crackdown on fentanyl manufacturing in China. The strips also fail to indicate the amount of fentanyl contained in a shot—just whether it contains any at all—which can leave people who still want to use the shot in question at a disadvantage.
The endorsed intervention comes as the CDC is reporting the “largest number of drug overdoses for a 12-month period ever recorded” between June 2019 and the end of May 2020. Already on the rise throughout 2019 and into the beginning of 2020, fatal overdoses appeared to accelerate, totaling 81,000 deaths as the COVID-19 crisis isolated people and disrupted drug economies.
“The increase in overdose deaths is concerning.” said Dr. Deb Houry, director of CDC’s National Center for Injury Prevention and Control, in a press release. “CDC’s Injury Center continues to help and support communities responding to the evolving overdose crisis. Our priority is to do everything we can to equip people on the ground to save lives in their communities.”
Financing the provision of test strips is exactly one way the CDC could support its own recommendation.
It’s unclear the role the CDC will play in making widely-accessible drug-checking services a reality in the US but, thus far, it does not seem to be promoting them. At least one grant administered by the agency to regional health departments, Overdose Data to Action, explicitly prohibits the purchase of fentanyl test strips with grant money.
Financing the provision of test strips, which usually cost $1 each, is exactly one way the CDC could support its own recommendation. “Most harm reduction services are struggling even more in light of COVID-19 and state and local budget shortfalls so that we need more financial support to ensure that these programs are able to provide a full array of services, including drug checking and distributing fentanyl test strips,” said Vakharia.
As it stands, the recommendation appears to be mostly symbolic. “Historically, we know that statements and recommendations by federal entities can only so go so far to actually change conditions on the ground,” said Vakharia, “unless they change policies and provide financial supports.”
Although Vakharia said drug checking would “undoubtedly lower the number of overdose deaths,” she also emphasized the need for far more radical interventions. “It is an imperfect solution and strategy to stay safe in the context of drug prohibition and an unregulated drug supply. While drug checking is essential, it can only do so much in light of the fact that people who use drugs need a safe supply.”
The CDC’s drug-checking recommendation comes alongside other harm reduction recommendations. Among them, making buprenorphine and other opioid use disorder medications easily accessible to patients; increasing overdose prevention access and ensuring people who use drugs have take-home naloxone; connecting participants with additional care; and considering the expansion of peer health navigator programs.
*DPA has previously provided a restricted grant to The Influence Foundation, which operates Filter, to support a Drug War Journalism Diversity Fellowship.
Photograph of fentanyl test strip by Filter staff.




Show Comments