In elementary school, my best friend Celina wanted to be a doctor when she grew up. She loved science, gave her parents impromptu lectures on the orbits of the planets, gathered interesting leaves and inspected wriggly insects under damp clay pots. There was only one problem—Celina struggled with math. To inspire her to improve her grades, our math teacher would whack her on the back of the head with the sharp edge of a ruler whenever she made an error in class. By the time I moved away the following year, Celina no longer wanted to be a doctor.
Our math teacher’s approach is an example of the operant conditioning modality of positive punishment. It discourages a behavior by adding (hence the “positive”) a noxious stimulus, and the subject of that stimulus then learns to avoid it by changing the behavior in question. This cycle is familiar to many survivors of abuse, relationship violence and bullying. It’s recognizable in even society’s most mundane forms of positive punishment, like parking tickets.
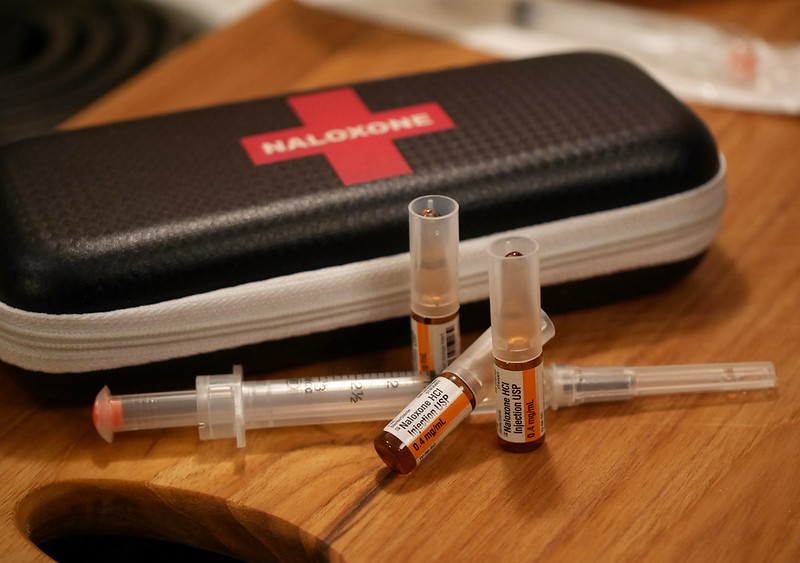
In April, the Food and Drug Administration approved Kloxxado, an 8 mg naloxone nasal spray. Kloxxado is similar to the much more recognizable Narcan, which is a 4 mg nasal spray. Both are single-dose products of the same silhouette and general size. But while opioid users are widely familiar with Narcan’s standard 4 mg, Kloxxado’s double-strength dose is unprecedented.
By contrast, single-dose vials of intramuscular naloxone found in ambulances or on pharmacy shelves are 0.4 mg. Just one or two doses injected into a muscle have remained consistently effective even in our increasingly fentanyl-saturated market. Kloxxado produces a maximum blood plasma concentration more than 11 times what’s usually sufficient.
Even with the proliferation of novel opioids, there is no compelling evidence for an 8 mg sledgehammer.
The rollout of an 8 mg naloxone product was probably inevitable. Rates of fatal overdose have increased exponentially over the past decade, and reached a catastrophic zenith under the pandemic as people who use drugs were forced to isolate, source their supply from unfamiliar sellers and adjust to dramatically reduced hours and services among syringe service programs (SSP).
Even before the pandemic, aggressive prohibition was relentlessly splintering the composition of the state-banned drug supply. What’s sold as heroin these days is likely to contain any number of names in a long list of unfamiliar, polysyllabic molecules—flualprazolam, furanylfentanyl, isotonitazene. These names are unfamiliar to most of us, and unfamiliarity breeds fear.
But even with the proliferation of novel opioids, there is no compelling evidence that supports a need for an 8 mg sledgehammer. The 4 mg Narcan already achieves a high plasma concentration and comes in a standard two-pack; in the event that the second dose is needed, it can be administered a few minutes after the first. But this hasn’t slowed the flood of misguided news stories of naloxone-resistant opioids that can take a cop down with mere incidental exposure. Panic builds, marketing opportunity arises and now we have Kloxxado. And on the horizon, another product that’s more potent still.
Currently under development for commercial rollout as a nasal spray, nalmefene is an opioid antagonist that works similarly to naloxone but clings to opioid receptors more tightly, for much longer. It was relatively unheard of before Opiant Pharmaceuticals pitched it as the answer to a 2017 National Institutes of Health call for “stronger, longer-acting formulations of antagonists” to combat the rise in fatal overdose. The resulting product will be around five times more potent than Narcan.
Naloxone revival can be a brutal experience. It throws the recipient into an abrupt whiplash from being high to being in withdrawal—bringing nausea, vomiting, pain, chills, sweats and diarrhea. In the hands of a skilled administrator, intramuscular naloxone can minimize this suffering because it can be dosed slowly and conservatively.
But gradual titration isn’t possible with nasal sprays—like Narcan, Kloxxado and the forthcoming nalmefene product—because the plunger delivers the entire dose in one push. This can make it easier for people without medical training to administer, and an easily taught intervention is usually for good public health. Except when outsized dosing comes into play.
It’s not just that naloxone doses of 8 mg or higher are unnecessary—they may be actively harmful.
It’s not just that naloxone doses of 8 mg or higher are unnecessary—they may be actively harmful. For opioid-tolerant users, waking up to agonizing pain can prompt the understandable desire to make it stop. The quickest way to do this would logically seem to be consuming an opioid.
Often what’s at hand will be the same batch that led to overdose only moments before. And because the naloxone will still be active in the brain for several hours, any opioids used in that time won’t bring the expected relief—pushing some people to use even greater amounts, out of desperation. So on top of the positive punishment effect training people to associate naloxone with misery, ultra-potent opioid antagonists could be poised to increase fatal overdose.
There are ways we can reduce this harm; take the handful of EMS programs that offer post-naloxone buprenorphine to ease withdrawal. But it’s much more common for health care providers to treat people who use state-banned drugs with hostility, contempt and lack of empathy. If we embrace ultra-potent opioid antagonists, we send yet another signal to drug users that their suffering is incidental, as is whatever happens to them after we pack up and leave.
It’s not hard to imagine Kloxxado and the nalmefene product enjoying a warm welcome from law enforcement. Bureaucrats, too, may appreciate these products as an easy out when speaking about the overdose crisis; they can assure the public that they’re funding the strongest possible interventions. But comfort of police officers and public officials is immaterial to this crisis. We must consider the risk of ultra-potent opioid antagonists functioning as positive punishment—teaching the people at highest risk of overdose that overdose antidotes are simply not worth the misery.
Before reaching over Narcan for Kloxxado, or Kloxxado for nalmefene, talk to the populations who are going to be on the receiving end. They can tell you that in most cases, no good will come from use of these products. Tread cautiously.
Photograph via Flickr/Creative Commons 2.0
The author would like to thank Dr. Lucas Hill at The University of Texas at Austin College of Pharmacy for his feedback and guidance in developing this piece.