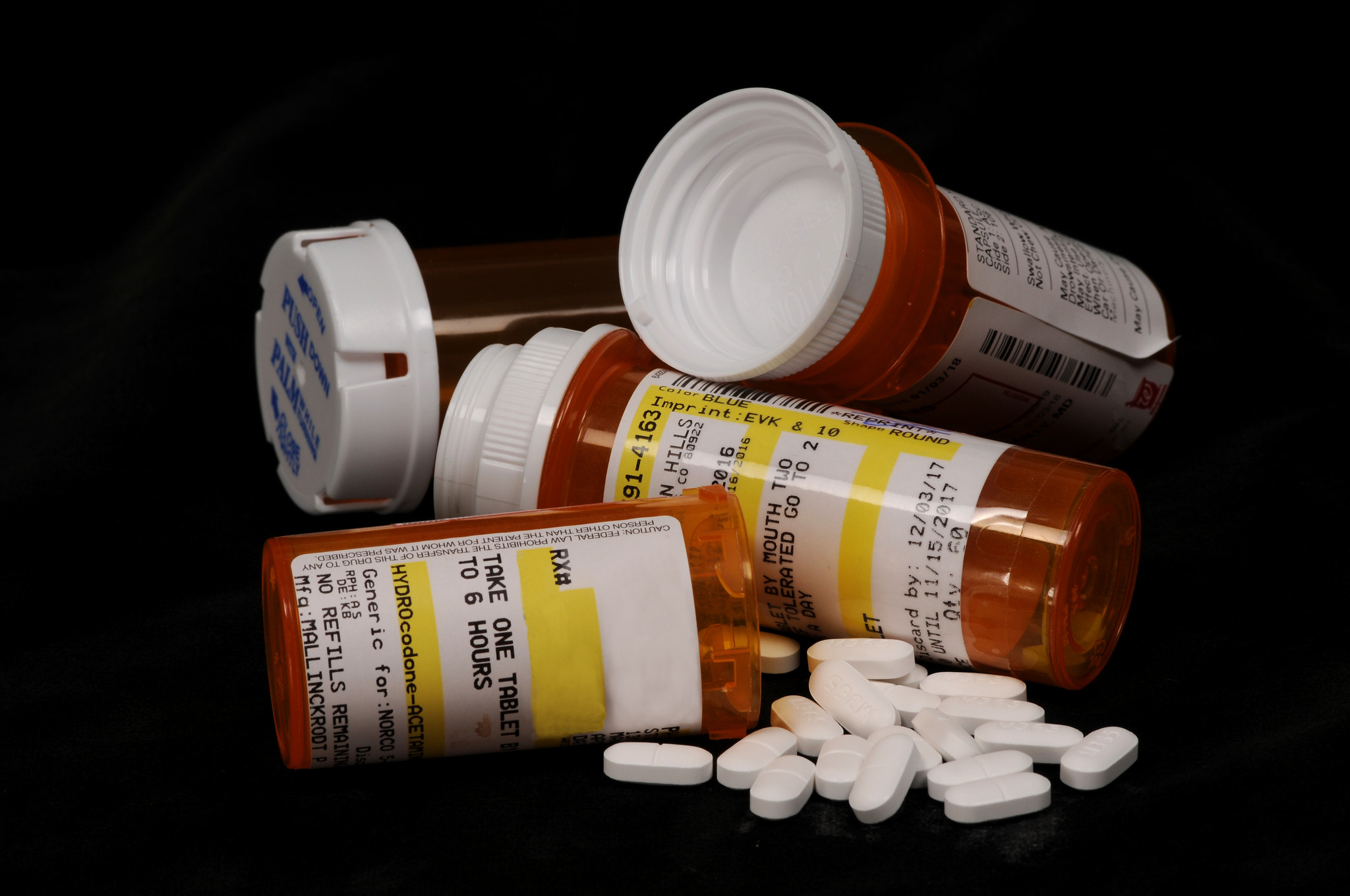
A rarity among academic papers, a new piece of research proposes models for legalizing opioids for non-medical use. A glut of research already surrounds the benefits of decriminalization and medicalized safe supply. But now, two Canadian researchers have offered three potential frameworks that would allow people to access opioids for things like recreation—though in the article itself, published in the International Journal of Drug Policy, the authors avoid using that term.
According to Mark Haden, who co-authored the paper with Brian Emerson and is a professor at the University of British Columbia’s school of Population and Public Health, both the prohibition of opioids and the commercialization of opioids for medical use have contributed to the overdose crisis. Because of this, and the other societal ills that prohibition brings, it’s important that governments find new ways to regulate the drugs.
“What we believe is that medicalization of opiates may not be the best way to improve public health,” Haden told Filter.
Harm reduction experts speaking to Filter about the paper say it could represent a step forward. But some people who use drugs may not want to engage with their country’s medical systems—to the extent they would still have to under the frameworks. And it’s vital that people who use drugs are engaged in any decisions surrounding potential legalization.
The first model involves a process of mandatory training and personal licensing for people who want to use opioids.
The paper deals explicitly with Canada, but, Haden noted, the US and other jurisdictions sometimes take cues from the country when it comes to drug policy. The paper further proposes changes in prescribing for medical use—like the creation of multi-disciplinary teams able to prescribe a broader range of opioids for issues like pain or addiction—but its main focus is on non-medical use.
Haden emphasized that the paper—which cites and analyzes scores of articles on opioids, addiction and public health—doesn’t claim any one of its three suggested frameworks is better than the others.
The first model involves a process of mandatory training and personal licensing for people who want to use opioids. Functionally, a person would learn the ins and outs of opioids and how to use them safely and unproblematically. During this period, they could only use their money to buy the drugs from staff in supervised consumption zones—Haden suggests existing medical clinics and safe consumption sites could fill in here.
After this kind of probationary period, if a person demonstrated they can use opioids safely, they could begin to take the drugs home. This model also comes with some government oversight—each person’s opioid use would be tracked, and there could be government interventions if it is deemed to become too problematic.
The second model is similar to the first, but without the government tracking. However, a person’s license could be “deactivated” if a staff member at the place of purchase notices their drug use is negatively impacting other aspects of their lives—like employment, or friends and family. The person would then be directed to the medical system to access their drugs and other resources to get the other elements of their lives functioning again.
The third model is roughly the same as the second, but the training to get a license would be optional. There would be no government tracking, but a person could still get referred to the medical system.
The authors say that the different levels of health care or government oversight could help ensure people using the drugs get the supports—employment, housing, health, etc.—they may need during their use. Haden also noted that the government oversight option doesn’t include the government telling people to stop using opioids outright.
“There are different levels of oversight,” he said. “It’s about how functional a person is in this world.”
The paper also notes that there could be a difference in terms of regulation between weaker opioids, like poppy tea, and stronger ones, like heroin. It further suggests that a licensing model could potentially also allow people to grow poppies for the sake of making their own poppy tea. (It should be noted that the amount of psychoactive alkaloids can vary from plant to plant.)
According to Haden, these models would allow people access to opioids of a known source and dosage, which, as a form of safe supply system, could reduce the number of opioid-related deaths. By simultaneously providing access to sterile syringes and other supplies, these strategies could also reduce transmissions of HIV and other blood-borne diseases. He also said that this strategy could help stem the flow of money to organized crime, though for this to work, the opioids would need to be priced as cheap as, or cheaper than, illicit sources.
“A lot of the criminal behaviour around drugs has nothing to do with drugs,” he added. “It has to do with the fact that drugs are illegal.”
Feedback From Harm Reductionists
Filter reached out to some harm reduction experts to ask for their reactions to Haden and Emerson’s proposals.
According to Steve Alsum, executive director of the Grand Rapids Red Project, a harm reduction provider in Michigan, their models have merits, but there are a few gaps. For one, people in rural areas who use opioids regularly or have an opioid use disorder would experience logistical problems if required to get to a clinic or other location frequently.
Further, the people who end up accessing opioids through the paper’s proposed medical channel might get left behind, Alsum said. People who use drugs regularly face stigmatization when interacting with the health care system, he added.
The paper notes that the multi-disciplinary teams involved in the medical pathway would include “allied health professionals,” and should be “guided by a trauma-informed approach.” All the same, Alsum said, people might be hesitant to get drugs from health care workers, and could end up buying unchecked drugs from illicit sources instead.
“Certainly, this is a step in the right direction from what we have right now,” Alsum concluded. “But I think there could still be big gaps in that because of the stigma … folks experience when they’re accessing medical services.”
Some people may be wary of obtaining or carrying a license that identifies them as a recreational opioid user.
According to Jess Tilley, executive director of the New England Users Union and the co-founder of HRH413, some people may also be wary of obtaining or carrying a license that identifies them as a recreational opioid user. But she also noted that having a legalized form of non-medical opioid use might decrease stigmatization.
Tilley also floated the idea of extending the training described in the models to friends and family members of people who use opioids. “I don’t think the training should just be for the individual using drugs. That’s going to break down the stigma,” she said.
Tilley said that the frameworks outlined in the paper could be modified in ways that might work better for people who use drugs.
First, all of the decisions surrounding a legalized framework—like creating the training process—should at every stage involve people who actually use drugs, she said. As part of this, different demographics within the population that uses drugs—sex workers, people without homes, etc.—should be involved. Tilley also said that hosting any supervised consumption at different harm reduction operations, rather than in wholly clinical settings, might help put people at ease.
Official Silence, But a Growing Conversation
Filter reached out to the US Food and Drug Administration about the new paper, but the organization declined to comment. “Generally, the FDA does not comment on third-party research, but evaluates it as part of the body of evidence to further our understanding about a particular issue and assist in our mission to protect public health,” an email from the organization read.
Health Canada also declined an interview, but sent an emailed response to Filter, noting some of the government’s strategies in reducing overdose deaths, such as the Good Samaritan Overdose Act, and allowing and funding safe supply programs.
“Substance use is a health issue, not a moral one,” wrote Cole Davidson, spokesperson for Minister of Health Patty Hajdu. “The COVID-19 pandemic has compounded the impacts of the opioid crisis, and we cannot forget how it has impacted thousands of families in communities across Canada. We have lost too many Canadians to overdoses and all levels of government must redouble efforts to save lives.”
“This is a conversation that really needs to happen. There’s a lot of room for creativity and innovation.”
It’s unlikely that Canada, the US and other countries around the world will legalize opioids any time soon. But Jules Netherland, managing director for the department of research and academic engagement at the Drug Policy Alliance*, said she thinks that the paper is an interesting step forward. The big advantage of a legal, regulatory system, she noted, is that it creates a supply of drugs of a known dosage and purity. And governments and drug policy experts should start thinking about as many different options as possible, and conduct “interesting, healthy debate” about which may or may not work.
“It’s kind of amazing that we’re at a time where we can start to talk about the specifics of different models,” she said.
Other researchers and organizations have previously released reports on how to legalize and regulate other drug classifications. For example, the Transform Drug Policy Foundation published a document about regulating stimulants.
Netherland also suggested that, besides focusing on any particular model, policymakers and researchers should consider what kinds of principles should end up guiding regulation. Further, more study should be performed on the successes and failures of other forms of drug legalization, like cannabis, tobacco and alcohol.
“There’s a lot of room to explore options of models,” she said. “This is a conversation that really needs to happen. There’s a lot of room for creativity and innovation.”
* DPA previously provided a restricted grant to The Influence Foundation, which operates Filter, to support a Drug War Journalism Diversity Fellowship.
Photograph via Flickr/Creative Commons 2.0