Asian American and Pacific Islander (AAPI) New Yorkers saw the largest spike in overdose deaths of any racial group between 2017 and 2018, a time span in which overall fatalities fell—yet their numbers were excluded from the city’s 2018 official report.
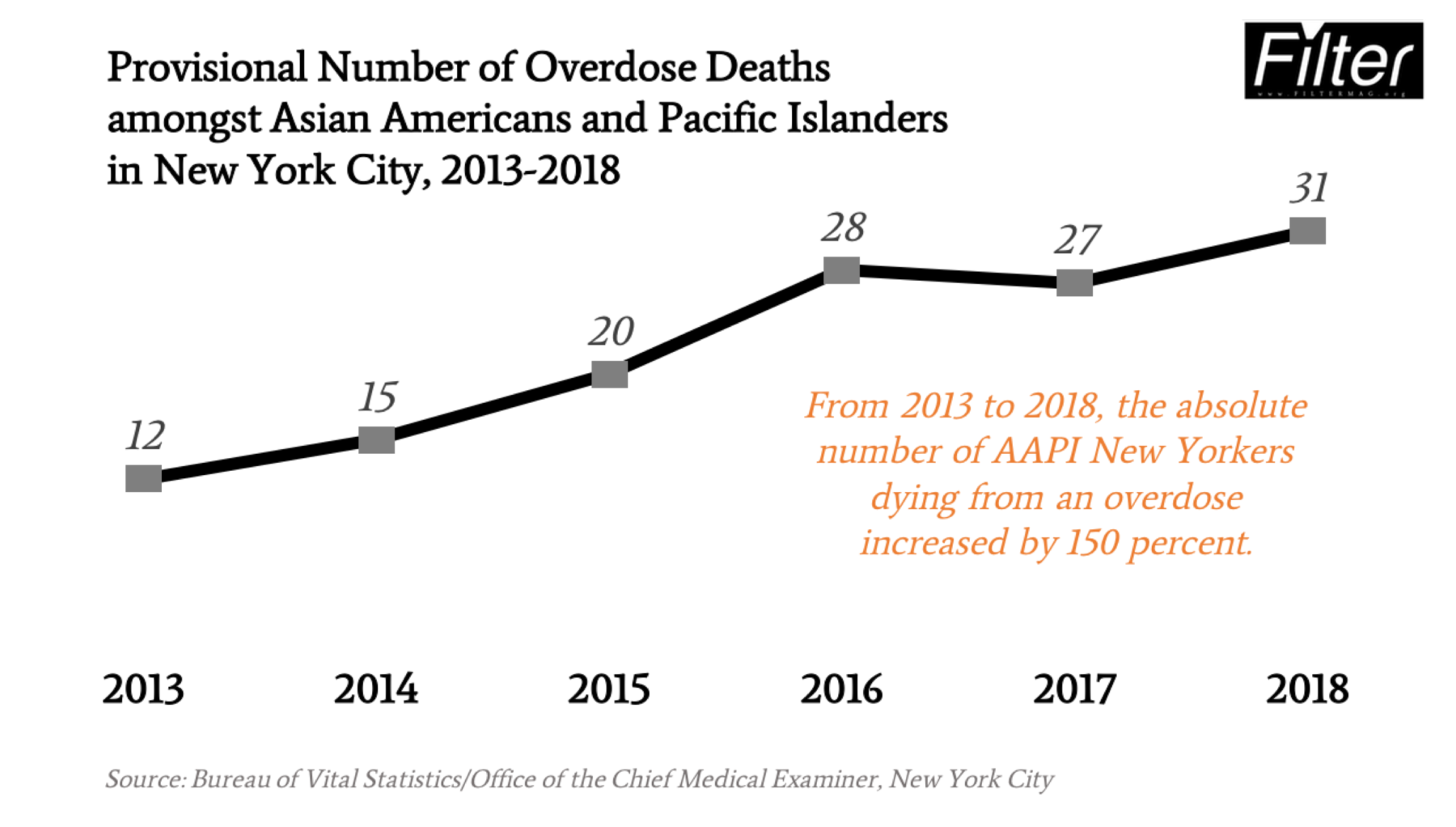
According to “suppressed” health department data obtained by Filter, the unintentional drug poisoning death rate for AAPI folks increased last year by 12 percent—a rate of increase more than double that of Latinx New Yorkers (5 percent), who experienced the only other increase for a racial group. AAPI New Yorkers still had a far lower absolute number of deaths (31) than other groups (white: 520; Latinx: 481; Black: 374).
The Department of Health and Mental Hygiene (DOHMH) did not publicly disaggregate the AAPI numbers when its report was published on August 26 due to the “low numbers” raising “concerns about anonymity,” a DOHMH spokesperson told Filter.
Dr. Kim Sue, the Harm Reduction Coalition’s medical director, noted to Filter that low absolute numbers can “make a percent rate appear higher,” though she added, “that doesn’t mean it’s not a problem.” Similarly, the health department spokesperson clarified that any overdose death “is one too many.”
Jason Tan de Bibiana, a Vera Institute researcher focusing on public health and criminal justice responses to drug use, is concerned about the lack of public acknowledgement for the worsening situation that AAPI New Yorkers who use drugs are facing.
“It was surprising that Asian New Yorkers were not a part of that data set that was presented publicly,” Tan de Bibiana told Filter. DOHMH has released other drug-related reports, like one on syringe exchange participants, that did include AAPI data. “Leaving out the information is a missed opportunity to raise awareness about the trends and the issue for Asian New Yorkers as well as the general public.”
But it can also bear material consequences. “Having this information available to public service-providers is really helpful for how they serve these populations in the city,” Tan de Bibiana explained. For example, AAPI people’s proportion of total deaths over the past few years has remained roughly stable (while deaths among white people, for example, have fallen as a percentage of the whole), something that Tan de Bibiana believes could “point to gaps in awareness and gaps in service delivery.” Yet specific AAPI death counts between 2013 and 2018, as seen by Filter, have not been accessible to public service providers.
This could be contributing to the idea that the harms of drug use are not a problem for AAPI New Yorkers, which itself is adjacent to the racist “model minority” myth.
AAPI people have been mostly left out of the conversation and sidelined from resource allocation by grassroots syringe exchanges in the city. As Filter recently reported, the Lower East Side Harm Reduction Center (LESHRC) has not committed the necessary resources, like staff with competence in speaking Cantonese, to ensure that drug users living in Chinatown, where LESHRC is located, have the opportunity to learn about and access life-saving tools, like naloxone.
In response to these barriers discovered by Filter, the health department spokesperson said that DOHMH “will ensure that the programs have harm reduction education materials in various languages, as well as the capacity to serve all clients.” The Alliance for Positive Change, the organization that operates LESHRC, did not respond to Filter‘s previous request for comment.
DOHMH is planning to make additional interventions. It now intends to “present the total number of drug overdose deaths in our report among Asians moving forward,” stated the spokesperson, citing the “slight” increase in fatalities. By presenting the numbers, DOHMH will be taking a step that could encourage more awareness amongst organizations who serve drug users and those that already serve the AAPI community—the latter of which, for Sue, are “critical” in “deliver[ing] harm reduction in ways that resonate” with the demographic.
But AAPI drug-specific data will still be subject to suppression for similar anonymity concerns. Tan de Bibiana points out that “overdose death is only one metric,” noting that, while it is “obviously the most tragic and impactful, we don’t have the data on the drugs being used, or points of prevention leading up to these deaths. The more data that’s available will be helpful in reducing the harms associated with drug use.”
For now, though, the data, for Tan de Bibiana, “brings up more questions than answers.”
Graphic of provisional number of overdose deaths amongst AAPI in New York City, 2013-2018; by Filter