Disparities in local availability of harm reduction resources could mean life or death for people who use opioids, suggests Canadian research. Places in Canada that lack accessible naloxone or safer consumption spaces (SCS) tend to have higher rates of overdose fatalities, as you might expect.
“If we go back to the idea that the number of overdose deaths is … concentrated in BC, Ontario, and Alberta, then that aligns with what we’re seeing in matching the response,” said Rebecca Jesseman of the Canadian Centre on Substance Use and Addiction.

Illustrating this, the Canadian government has mapped the opioid-related services available in each province:
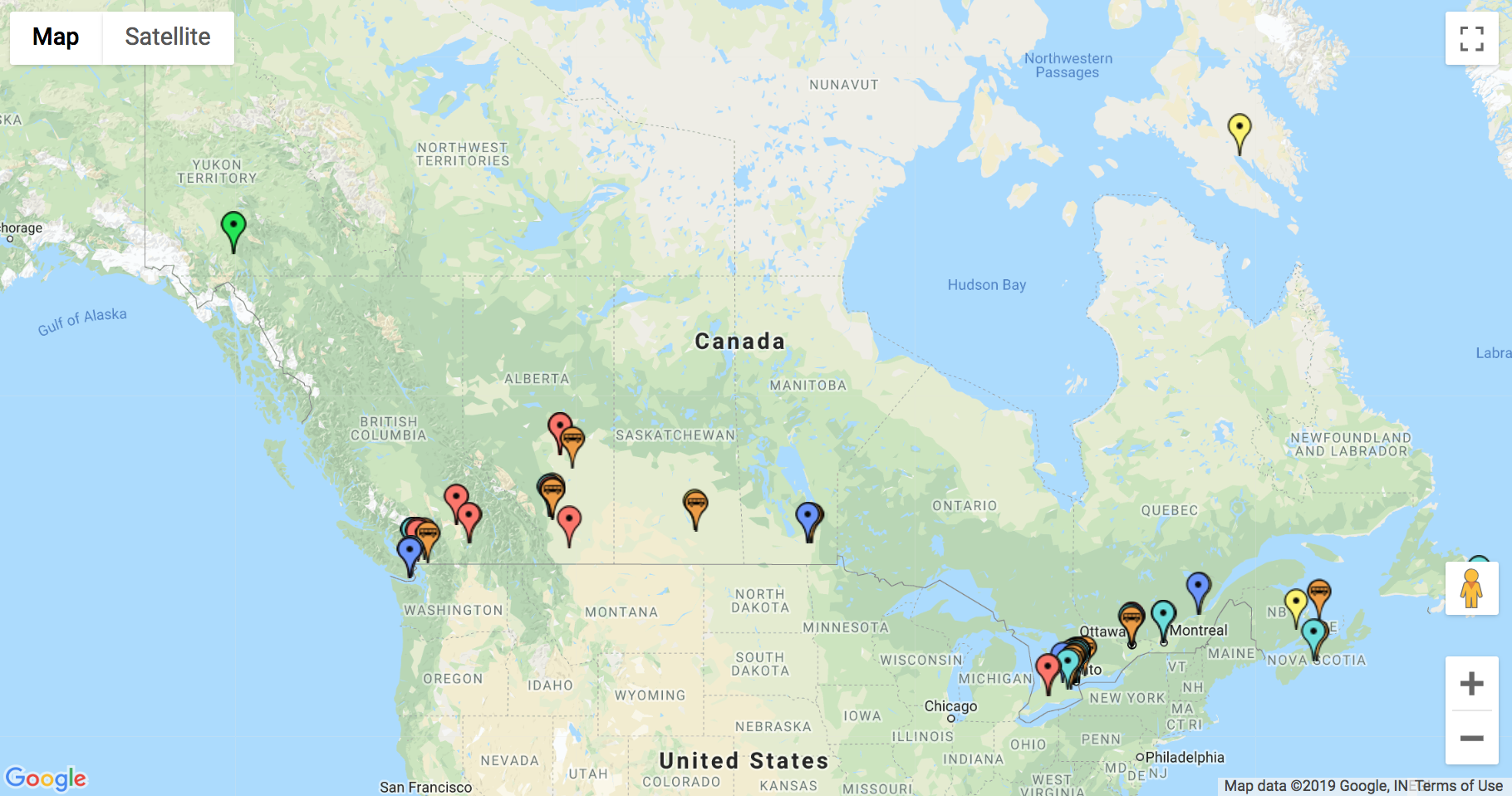

However, resources’ placement within states is often far from ideal. In British Columbia, for example, most resources are concentrated in the Vancouver metropolitan area, famously home to Insite, the first legal SCS in North America. But according to British Columbia Centre for Disease Control data, the central region of the province has had some of the highest rates of illicit drug overdoses in the past year.
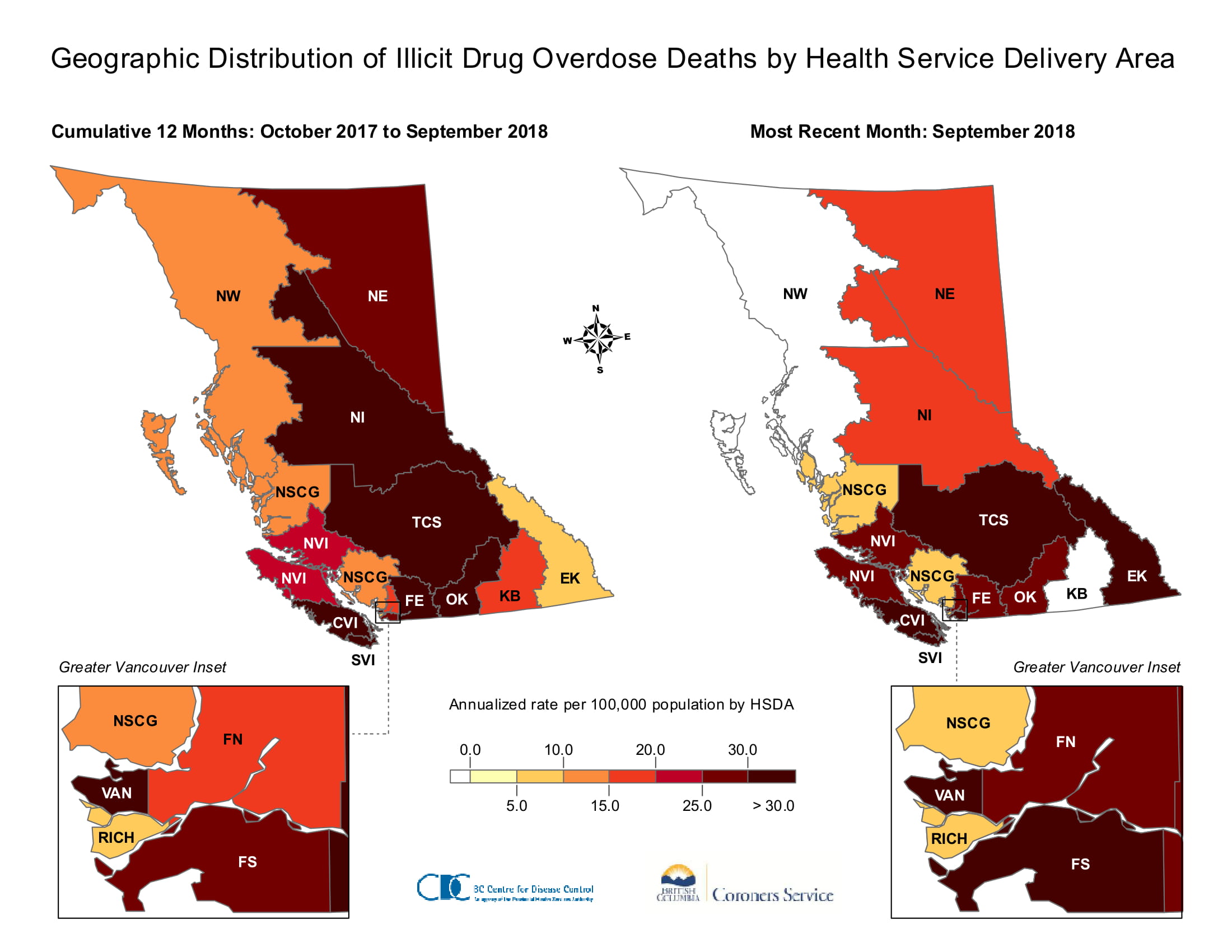
Such geographic disparities frequently stack up against marginalized people. “We have very limited services that are specifically addressing the needs of First Nations people, for example,” says Jesseman. First Nations communities tend to be more heavily distributed outside of major metropolitan areas, and therefore have less access to harm reduction services.
Canada saw a total of 2,066 reported opioid-related deaths between January and June 2018, according to the Public Health Agency of Canada.



